Bunion Treatment in Frisco
What are bunions?
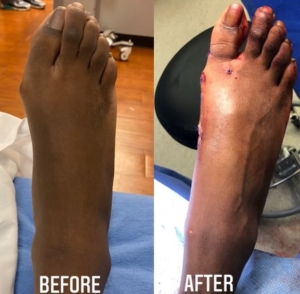
Bunions are bumps or prominences on the inside of the foot near the great toe joint. Although we just think of a bunion as the bump on the side of the foot, there is more occurring than just that. When a bunion develops, the big toe starts to angle or lean towards the second toe. The large toe joint becomes out of alignment leading to the visible bump. The medical term for this condition is Hallux Valgus. Bunions start small and gradually progress with time. Bunions are not always painful, however, the larger they become the more likely they are to become painful especially with wearing shoes. Since the big toe drifts over towards the second toe, bunions (hallux valgus) can often lead to the development of hammertoes and calluses.
What are the symptoms of bunions?
- Pain at big toe joint
- Redness noted at the site of the bunion
- Pain with snug shoes/ high heels
- Numbness or burning pain as nerves can become entrapped between the bone and skin
- Stiffness
What causes bunions?
Bunions are typically a result of a person’s foot structure, which is hereditary. Although genetics are the cause of bunion (hallux valgus), certain risk factors such as wearing ill-fitting, unsupportive shoes may lead to progression and worsening of the deformity. Bunion deformities are more common in women and over the age of 60.
What are treatment options for bunions?
Nonsurgical options will not fix the bunion but will alleviate symptoms and slow progression. These include:
- Orthotics to provide proper arch support and promote a better gait pattern. These will help slow down the progression of the bunion.
- Supportive shoes with a wider toe box to accommodate the bunion
- Bunion padding/shields/taping
- NSAIDs for acute pain
- Toe separators to take pressure off of the second toe
- Cortisone injections are an option to alleviate acute pain and nerve irritation
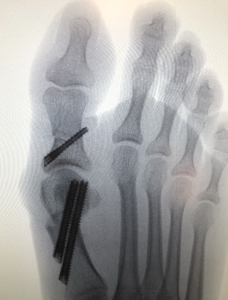
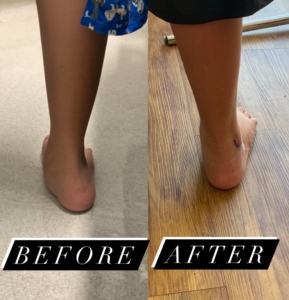
If conservative treatment options fail, surgical intervention is the next step. There are many different types of surgical procedures depending on the severity of the bunion. Prior to surgery, we will need to take x-rays to help in surgical planning. Often these surgeries, called bunionectomies, require cutting the bone and realigning it as well as shaving off any prominent bunion. At Star Foot & Ankle Specialists, we also offer minimally invasive surgery. Minimally invasive surgery results in minimal scarring and often leads to a quicker recovery.
If you are suffering from bunions click HERE to make an appointment to come see us and find the best treatment plan for you!

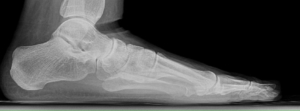
 Heel pain is often caused by a very common condition called plantar fasciitis, which is inflammation of the plantar fascia. The plantar fascia is a ligament that starts on the heel bone, runs across the bottom of the foot, and ends near the base of the toes. This means that the plantar fascia acts as an arch support.
Heel pain is often caused by a very common condition called plantar fasciitis, which is inflammation of the plantar fascia. The plantar fascia is a ligament that starts on the heel bone, runs across the bottom of the foot, and ends near the base of the toes. This means that the plantar fascia acts as an arch support.


