(972) 559-0051
By clicking SUBMIT you consent to receiving SMS messages
Messages and Data rates may apply. Message frequency will vary
Reply Help to get more assistance
Reply Stop to Opt-out of messaging

Flat feet are very common in children — but not all flat feet need treatment. Here’s how to know the difference.
Flat feet — when the arch of the foot is low or absent — are extremely common. Many people with flat feet have no symptoms at all. But for others, flat feet contribute to foot pain, leg fatigue, knee problems, and difficulty with prolonged activity.
Nearly all infants are born with flat feet. Arches typically develop between ages 3 and 6. If a child still has significantly flat feet after age 6 — especially with complaints of foot pain, fatigue, or awkward gait — a podiatric evaluation is appropriate.
Signs to watch for in children:
The good news: Most pediatric flat feet respond very well to supportive orthotics and do not require surgery.

Not all flat feet are the same — an evaluation helps determine whether treatment is needed based on your foot type and symptoms.
Adult-acquired flat foot (fallen arch) most commonly results from posterior tibial tendon dysfunction (PTTD) — a gradual failure of the tendon that supports the arch. It is more common in women and people over 40.
Symptoms include pain along the inner ankle and arch, swelling, difficulty standing on tiptoe, and progressive deformity of the foot. Early treatment is critical — advanced PTTD can lead to arthritis and may require surgical reconstruction.

Custom orthotics are the most common and effective treatment for flat feet in both children and adults — no surgery required in the vast majority of cases.
Q: Are flat feet a disability?
A: Flat feet themselves are not a disability, but symptomatic flat feet that limit function can be significantly disabling without proper treatment.
Q: Can flat feet be corrected in children?
A: Custom orthotics can support proper development and relieve symptoms. Most children do not need surgery.
Q: Do I need orthotics if my flat feet don’t hurt?
A: Not necessarily. Asymptomatic flat feet in adults often require no treatment. An evaluation can determine if preventive care is appropriate given your activity level and foot structure.
Frisco Foot & Ankle Specialists offers prompt appointments for acute injuries. Call (972) 559-0051.
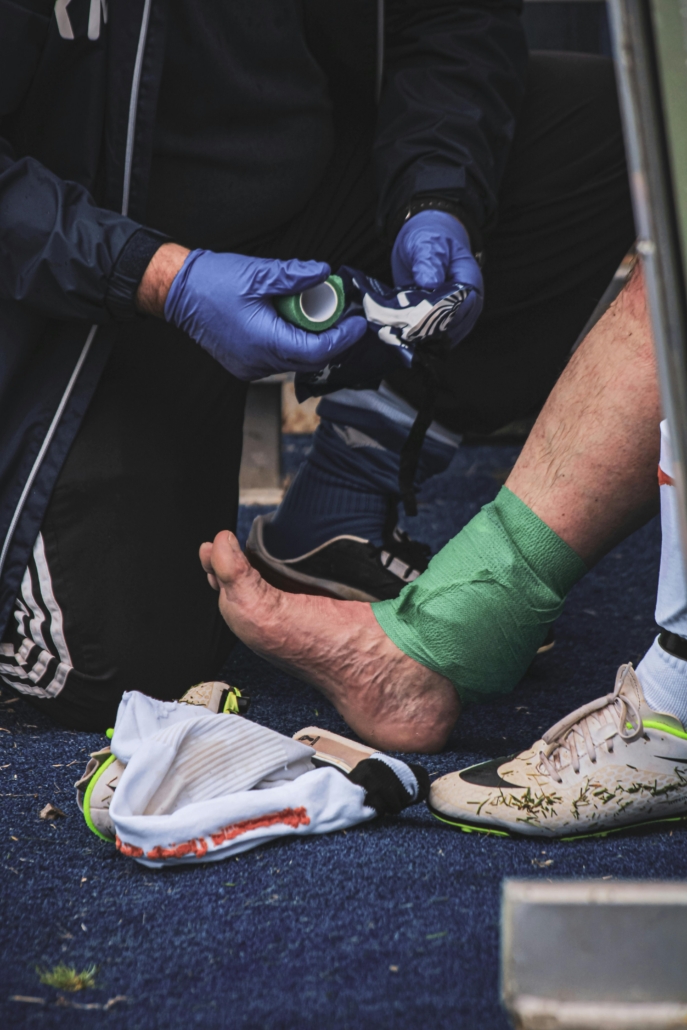
What you do in the first 48 hours after a foot or ankle injury can significantly affect your recovery.
Foot and ankle fractures are among the most common orthopedic injuries — and also among the most mismanaged, because patients either delay seeking care or go to an ER that isn’t equipped for specialist follow-up. Getting the right care quickly matters for how well and how fast you recover.

The 5th metatarsal (outer edge of the foot) is one of the most commonly fractured bones — often injured when rolling the ankle.
Important: Being able to walk does not rule out a fracture. Many fractures, including some serious ones, remain weight-bearing.
If the foot or ankle is severely deformed, the skin is broken, or you cannot bear any weight at all, go to the ER first. For most fractures — including stress fractures, toe fractures, and stable ankle fractures — a same-day or next-day appointment at Frisco Foot & Ankle is faster, more comfortable, and provides better continuity of care than a hospital emergency department.
We have in-office digital X-rays and can have you diagnosed, immobilized, and in a treatment plan within your first visit.
Q: How do I know if my foot is broken or just sprained?
A: You often can’t tell without an X-ray. Both can cause swelling and significant pain. When in doubt, get it evaluated.
Q: How long does a foot fracture take to heal?
A: Most uncomplicated foot fractures heal in 4–8 weeks. Ankle fractures and complex injuries may take 3–6 months for full recovery.
Q: Can I drive with a foot fracture?
A: Generally no, especially with fractures of the right foot, ankle, or any injury requiring a boot or cast. Your doctor will advise you based on your specific fracture.
Frisco Foot & Ankle Specialists offers prompt appointments for acute injuries. Call (972) 559-0051.

Most people wait far too long to see a podiatrist. If any of these five signs sounds familiar, it’s time to make the call.
Most people wait too long to see a podiatrist. Foot and ankle problems rarely resolve on their own — and the longer you wait, the more complex (and expensive) treatment often becomes. Here are five signs it’s time to make an appointment.
Foot and ankle pain that persists beyond two weeks is your body signaling that something isn’t resolving on its own. This includes heel pain, arch pain, ball-of-foot pain, or any joint discomfort that you’ve been “walking off” or managing with ibuprofen.
Limping, avoiding your heel, or unconsciously shifting weight are signs your body is compensating for an injury. These compensatory patterns often create secondary problems in the knees, hips, and lower back if left unaddressed.

At Frisco Foot & Ankle Specialists, patients consistently describe feeling heard, unhurried, and genuinely cared for.
Every person with diabetes should have an annual podiatric exam. Diabetic neuropathy and circulation issues make foot problems disproportionately dangerous — and most patients don’t realize how serious a small wound or ingrown nail can become.
Toenail discoloration, thickening, ingrown nails, warts, and persistent calluses are all treatable conditions. Many patients live with these for years unnecessarily. Effective, comfortable treatment is usually straightforward.
These symptoms can indicate peripheral neuropathy, nerve compression, or circulatory issues. They should always be evaluated — both to identify the cause and to rule out conditions requiring prompt attention.
Q: What does a podiatrist treat?
A: Podiatrists specialize in all conditions of the foot and ankle, including fractures, tendon injuries, skin and nail conditions, nerve conditions, arthritis, and surgical correction of structural problems like bunions and hammertoes.
Q: Do I need a referral to see a podiatrist?
A: Most insurance plans do not require a referral for podiatric care. Call your insurance to confirm, or contact our office and we’ll help verify your benefits.
Q: Is a podiatrist a real doctor?
A: Yes. Podiatrists (DPM — Doctor of Podiatric Medicine) complete a 4-year podiatric medical school followed by a surgical residency program, with optional fellowship training in subspecialties like foot and ankle surgery.
Q: How do I make an appointment at Frisco Foot & Ankle Specialists?
A: Call (972) 559-0051, book online at friscofoot.com, or use our Zocdoc scheduling link for real-time availability.
Frisco Foot & Ankle Specialists serves patients of all ages at 3550 Parkwood Blvd Suite 702, Frisco, TX 75034. We treat the full range of foot and ankle conditions with compassionate, individualized care.
You no longer need to feel embarrassed to wear open-toe shoes and sandals – or just go barefoot – because of toenail fungus or discoloration.
Frisco Foot & Ankle Specialists is the area’s leader in restoring nails back to health, providing a natural and luminous appearance.
The Remy Class IV laser therapy is one of the most safe and effective ways to treat toenail fungus (onychomycosis)!
Laser therapy penetrates the nail bed and kills the fungus living underneath the nail – without pain and without any harmful side effects.
When the colony of fungus under the nail is “attacked” by the laser, the elements that make it grow and thrive are destroyed. This allows your nail bed to begin growing new, healthy nail. Nails that won’t give you feelings of discomfort or embarrassment!
Laser therapy is a quick and easy treatment allowing patients to relax during the procedure.
SCHEDULE A LASER CONSULTATION.
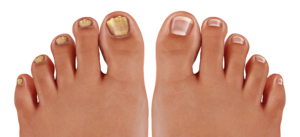
Fungal foot infections. They can create major discomfort and even embarrassment. They are also EXTREMELY COMMON; affecting millions of people each year.
Additionally, fungus is easily spread. Individuals with fungus may have contracted it through shared bathroom space, public locker rooms, showers, and pools, shared clothing or shoes, even carpeting.
For some, fungus is simply genetic. When this is the case, treatment can become even more difficult given the likelihood of reoccurrence.
One of the most prevalent types of fungal foot infections directly affects your toenails. This type of condition is known as onychomycosis.
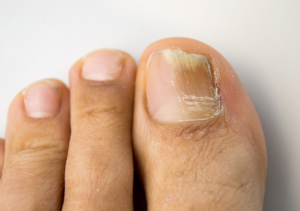
onychomycosis with fungal nail infection
You may have onychomycosis if you notice any of the following symptoms:
It’s not uncommon to feel discomfort and embarrassment due to the unsightly appearance and these symptoms of onychomycosis.
Fungal nail affects nearly 10% of the US population.
While many find the condition to be, simply, an eye sore, fungal nail can also lead to a larger problems incuding:
Individuals with diabetes are also more susceptible to fungal nail given their compromised immune systems.
Laser therapy offers an effective, safe option for treating fungal toenail without the side effects of many oral medications.
For more information visit FRISCO FOOT & ANKLE SPECIALISTS.
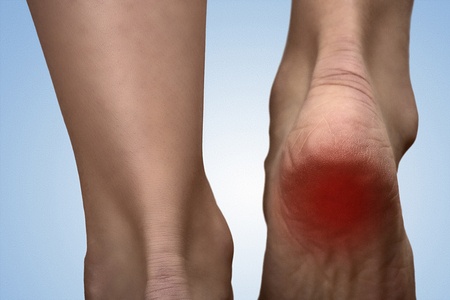
Everyone’s pain is different. Dr. Gary Heredia and Dr. Morgan Zellers of Frisco Foot & Ankle Specialists will diagnose and treat your unique pain – whether it’s in the heel, arches, ball of your foot and/or toes – getting you back to your daily routine with comfort and ease!
The Remy Class IV laser therapy is one of the most safe and effective ways to treat various conditions that cause foot and ankle pain! Laser therapy has a vast amount of benefits including:
SCHEDULE A LASER CONSULTATION AT:
FRISCO FOOT & ANKLE SPECIALISTS
With 26 bones in the foot alone, as well as major ligaments, tendons, joints, and nerves – it’s not surprising that millions of Americans suffer various types of foot and ankle pain.
The Remy Class IV laser therapy is used for the relief of pain, to accelerate healing and decrease inflammation.
When the light source is placed against the skin, photons penetrate several centimeters down and are absorbed by the mitochondria (the energy producing part of a cell). This energy results in the restoration of normal cell function.
The main goal of laser therapy is to stimulate the cell to perform its natural functions, but at an enhanced rate.
Laser therapy is a quick and easy treatment allowing patients to relax during the procedure. In contrast to “cold lasers,” which provide no feeling or sensation, high power diode laser therapy provides a warm, soothing feeling.
Some of the most common source of foot pain include:
Any one of these conditions can create chronic (long-term) pain or acute (short-term) pain.
For more information please visit our main site: FRISCO FOOT & ANKLE SPECIALISTS
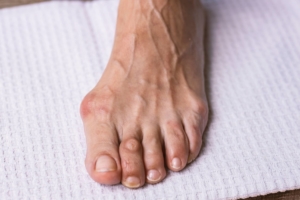
What are Tailor’s bunions?
A Tailor’s bunion (also commonly called a bunionette) refers to a prominent bone on the outside of the foot by the little toe. This bone is called the fifth metatarsal. A Tailor’s bunion can be asymptomatic. However, sometimes larger tailor’s bunions can be painful in shoe gear and with activity. There may also be an associated callus that forms from pressure which may cause pain.
What causes Tailor’s bunions?
What are treatment options for Tailor’s bunions?
Conservative treatment includes:
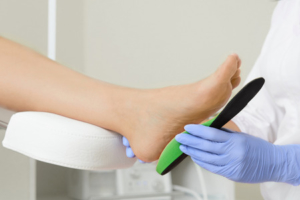
If conservative treatment fails, surgical intervention is an option. During surgery the bone is cut and realigned in better position to reduce the bony prominence. There are few different surgical techniques to correcting a Tailor’s bunion. This is typically dependent on xrays, foot structure, and activity levels.
In The Colony. Little Elm, Plano, and Frisco, we treat patients with Tailor’s bunions with an individualized and compassionate care plan. Click here to schedule an appointment with one of the podiatrists at Frisco Star Foot & Ankle Specialists!
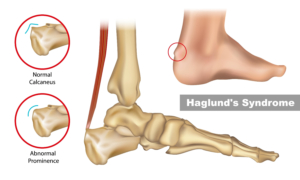
What is a Haglund’s Deformity?
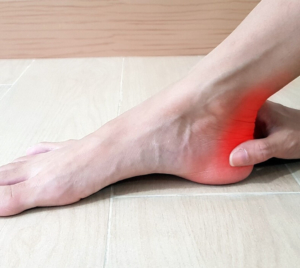
Here in Frisco, Texas podiatrists see a variety of foot and ankle conditions. One of the conditions we often see is called a Haglund’s deformity. A Haglund’s deformity is a prominent bony enlargement located at the back of the heel at the area where the Achilles tendon attaches. As the bony prominence enlarges, this can cause irritation to the Achilles tendon or bursitis (inflammation of a fluid filled sac between the tendon and the bone).
What causes a Haglund’s Deformity?
A Haglund’s Deformity is often referred to as a “pump bump” as it is commonly seen in females who wear pump like style high heels. Haglund’s deformities are also seen more commonly in those with very tight Achilles tendons and in those with high arches.
What are the symptoms of a Haglund’s deformity?
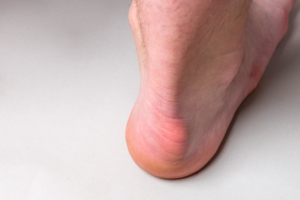
How to treat a Haglund’s deformity?
At Star Foot & Ankle Specialists, the podiatrists always start with conservative treatment options. For a Haglund’s deformity the following are conservative treatment options:
If conservative treatment options fail, we then consider surgical treatment options which include shaving the prominent bone.
If you are in Frisco, Plano, or Little Elm and are experiencing pain in the back of your heel, please give us a call to schedule an appointment with Dr. Heredia or Dr. Zellers or click HERE.
If you suffer from tight Achilles tendons or plantar fasciitis, stretching the Achilles tendon is super important. Below are some exercises that can help prevent injury and reduce symptoms.
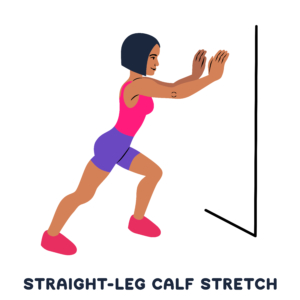
Wall Stretch

Calf Stretch with Towel or Exercise Band
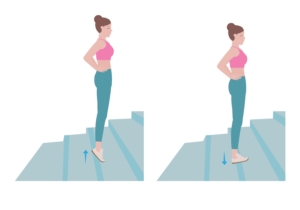
Stair Stretch

Plantar fascia Stretch
If you are located near Frisco, Plano, or Little Elm and are suffering from tight Achilles tendons or plantar fasciitis, click HERE to schedule an appointment with Dr. Heredia or Dr. Zellers at Star Foot & Ankle Specialists.

What is Achilles tendinitis?
In Frisco, we have an active population and with that carries the risk of injury. One of the more common injuries foot doctors see is Achilles tendinitis. The Achilles tendon is the tendon in the back of the lower leg that connects the calf muscle to the heel bone. This tendon is the strongest and largest tendon in our bodies. This tendon is imperative to walking, jumping, and running. When the tendon becomes inflamed, we start to develop Achilles tendinitis. The tendon can become inflamed at the insertion on the heel bone or higher up in the lower leg. When the tendon becomes inflamed at the insertion, there is sometimes a bony prominence called a Haglund’s deformity as well. We will discuss this in a future blog.
Symptoms of Achilles tendinitis include:
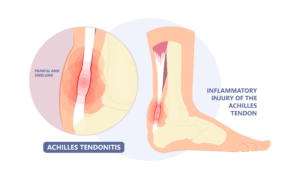
What are the causes of Achilles tendinitis?
Achilles tendinitis is often caused by overuse of the tendon. This is commonly seen in athlete’s that quickly increase their level of exercise without proper training. We often see Achilles tendinitis in weekend warriors, meaning those who may not be active regularly during the week but like to engage in more strenuous activities on the weekend. Achilles tendinitis can also be caused by tightness in calf muscles and lack of proper stretching. There are risk factors for Achilles tendinitis, including age and obesity. Achilles tendinitis is also more commonly seen in men.
How do you treat Achilles tendinitis?
How do I prevent Achilles tendinitis?
If you are having pain at the area of your Achilles tendon in Frisco, Little Elm, or Plano click HERE to make an appointment with your local foot doctors, Dr. Heredia or Dr. Zellers, at Star Foot & Ankle Specialists.